Assistant Professor Brandon Jutras, left, and research scientist and Edward Via College of Osteopathic Medicine medical student Mari Davis, right, in the lab at the Fralin Life Sciences Institute. Photo by Alex Crookshanks for Virginia Tech. CREDIT Credit Virginia Tech
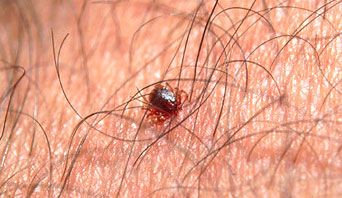
Lyme disease is carried by black-legged ticks and infects people when they are bitten and transmit the bacterium Borrelia burgdorferi. Black-legged ticks are especially common in the northeastern United States, and people are exposed to the ticks usually during outdoor activities. Warming temperatures and climate change have caused tick populations to explode and infiltrate more areas of the country, increasing the chance of getting the disease.
The Centers for Disease Control and Prevention estimate that 476,000 people are infected with Lyme disease every year in the United States.
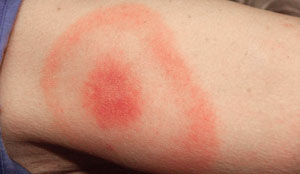
Early symptoms of Lyme disease are fever, headache, fatigue, and the possibility of a telltale bullseye rash at the bite site. If left untreated, the infection can spread to the joints, heart, and nervous system and cause debilitating long-term conditions including Lyme arthritis, carditis, and neuroborreliosis. Sometimes patients can still develop these symptoms despite proper therapy.
Brandon Jutras, assistant professor in the Department of Biochemistry in the College of Agriculture and Life Sciences, received a grant from the Global Lyme Alliance to improve diagnostic testing for all stages of Lyme disease and to develop new ways to treat patients when conventional treatment options have failed.
“We’re thrilled to partner with the Global Lyme Alliance, a longstanding organization dedicated to improving the outcome of patients suffering from this enigmatic disease,” said Jutras, an affiliated faculty of the Fralin Life Sciences Institute and the Center for Emerging, Zoonotic, and Arthropod-Borne Pathogens.
“This grant gives us the opportunity to try radical and innovative approaches like monoclonal antibody therapy. I applaud the Global Lyme Alliance for supporting this high-risk, high-reward research.”
When the infection is caught early and treated with antibiotics in the preliminary stages, patients often recover quickly without long-term effects. Patients who are treated in later stages of the disease may continue to suffer from ongoing symptoms, termed post-treatment Lyme disease.
“Late-stage complications of Lyme disease are due to how our immune system responds. With this funding, we are now able to test new ways to prevent our immune system from overreacting,” said Jutras.
Jutras recently made a discovery that may transform the way we understand acute and chronic symptoms of Lyme disease and Lyme arthritis.
“According to the CDC, cases of vector-borne diseases, such as Lyme disease transmitted from vectors to people, more than doubled between 2004 and 2018 in the United States. The Jutras lab already made a number of important discoveries about the bacterium that causes Lyme disease, B. burgdorferi,” said X.J. Meng, University Distinguished professor and interim director of the Fralin Life Sciences Institute.
“The Jutras lab recently discovered that the Lyme disease spirochete possesses a unique property in that it sheds peptidoglycan after it infects the human host. This discovery affords the opportunity for scientists to develop novel diagnostics by utilizing a unique biomarker for different stages of Lyme disease. This new grant from the Global Lyme Alliance will now allow the Jutras lab to further explore innovative therapeutic strategies against Lyme disease.”
Virtually all bacteria have a cell-wall component called peptidoglycan. But, as it turns out, the peptidoglycan of the Lyme disease bacterium is unique. They also shed it as they replicate. The B. burgdorferi peptidoglycan can be found in the joints of Lyme arthritis patients with post-treatment Lyme disease, and it can cause arthritis on its own.
The Jutras lab is developing methods focused on using peptidoglycan as a marker for new diagnostic tests for Lyme disease. Their research now includes using anti-peptidoglycan antibodies to improve existing diagnostics.
“An overarching goal of the Global Lyme Alliance is to foster transformative advances in the diagnosis and treatment of patients suffering from post-treatment Lyme disease. In pursuit of this goal, we are excited to fund the research of Dr. Jutras,” said Timothy J. Sellati, chief scientific officer of the Global Lyme Alliance. “The unique nature of B. burgdorferi peptidoglycan may lend itself to serving as a biomarker for bacterial persistence after treatment and as a target for removal as a means of minimizing or eliminating an underlying reason for persistent symptomatology.”
The Jutras lab is currently developing new ways to either mask or destroy lingering B. burgdorferi peptidoglycan to treat patients suffering from post-treatment Lyme disease.
“In a very short amount of time, Dr. Jutras has developed an impactful research program that engages several Virginia Tech students in Lyme disease research,” said Glenda Gillaspy, professor and department head of biochemistry in the College of Agriculture and Life Sciences. “Together, Dr. Jutras and his team are poised to use biochemical and molecular techniques to help innovate this field, and this recent award will provide significant and important support for the work.”

![Common Hidden Illnesses Explained [Infographic]](https://patienttalk.org/wp-content/uploads/2016/10/Hidden-illness-2.jpg)
