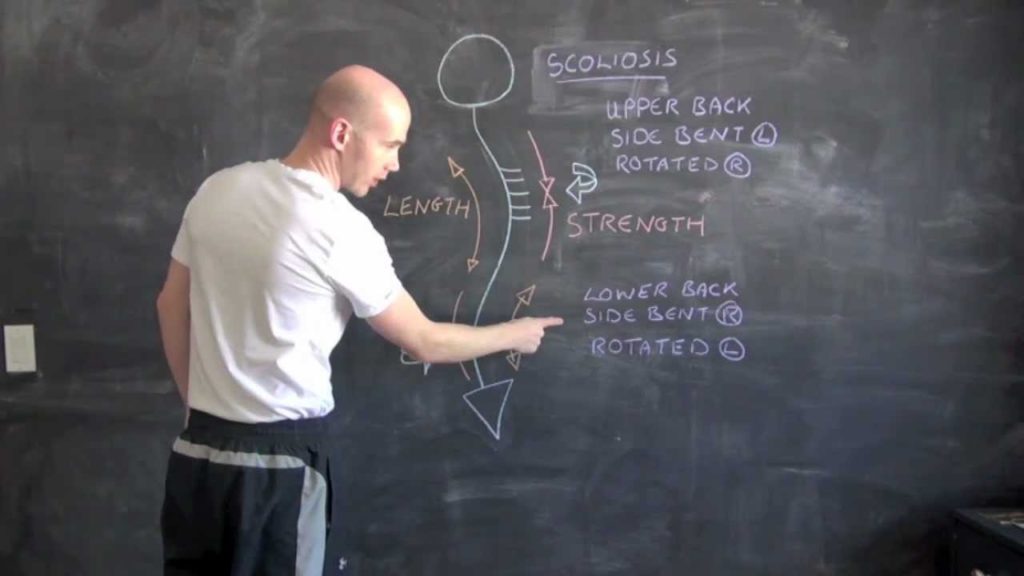
The spine is supposed to go straight up and down vertically. When people have scoliosis, the spine curves from side to side and may look like a “C” or an “S”. You can learn more by viewing this Houston minimally invasive spine treatment infographic.
Scoliosis
Living with Scoliosis: Telling the Emotional Story
Scoliosis – what are the signs and symptoms of Scoliosis?
Scoliosis is where the spine twists and curves to the side.
It can affect people of any age, from babies to adults, but most often starts in children aged 10-15.
Scoliosis doesn’t normally improve without treatment, but it isn’t usually a sign of anything serious and treatment isn’t always needed if it’s mild.
Symptoms of scoliosis
Signs of scoliosis include:
a visibly curved spine
leaning to one side
uneven shoulders
one shoulder or hip sticking out
the ribs sticking out on one side
clothes not fitting well
Some people with scoliosis may also have back pain. This tends to be more common in adults with the condition.
When to see your GP
See your GP if you think you or your child has scoliosis. It’s unlikely that there’s anything seriously wrong, but it’s best to get checked out.
Your GP will examine your back and can refer you to a hospital doctor for help with diagnosis if they suspect scoliosis.
An X-ray of your back will be carried out in hospital to check whether your spine is curved and how severe the curve is.
If you’re diagnosed with scoliosis, you should see a specialist to discuss treatment options.
Treatments for scoliosis
Treatment for scoliosis depends on your age, how severe the curve is, and whether it’s likely to get worse with time.
Many people won’t need any treatment and only a small number will need to have surgery on their spine.
Babies and toddlers may not need treatment as the curve might improve over time. A plaster cast or plastic brace may be fitted to their back to stop the curve getting worse as they grow.
Older children may wear a back brace to stop the curve getting worse until they stop growing. Sometimes surgery may be needed to control the growth of the spine until an operation to straighten it can be done when they stop growing.
Adults may need treatment to relieve pain, such as painkillers, spinal injections and, very occasionally, surgery.
It’s not clear whether back exercises help improve scoliosis, but general exercise is good for overall health and shouldn’t be avoided unless advised by your doctor.
Read more about treatments for scoliosis in children and treatments for scoliosis in adults.
Living with scoliosis
Most people with scoliosis are able to live normal lives and can do most activities, including exercise and sports.
The condition doesn’t usually cause significant pain or any other health problems, and tends to stay the same after you stop growing – see your GP if it gets any worse.
Having scoliosis or wearing a back brace can be tough and may cause problems with body image and self-esteem, particularly for children and teenagers.
You may find it useful to contact a support group, such as Scoliosis Association UK. These groups are a good source of information and support, and they may be able to put you in touch with other people in a similar situation to you.
Read more advice from Scoliosis Association UK about coping with scoliosis and scoliosis support.
Causes of scoliosis
In around 8 in every 10 cases, the cause of scoliosis is unknown. This is called idiopathic scoliosis.
Idiopathic scoliosis can’t be prevented and isn’t thought to be linked to things such as bad posture, exercise or diet. Your genes may make you more likely to get it, though, as it sometimes runs in families.
Less commonly, scoliosis may be caused by:
the bones in the spine not forming properly in the womb – this is called congenital scoliosis and is present from birth
an underlying nerve or muscle condition, such as cerebral palsy or muscular dystrophy – this is called neuromuscular scoliosis
wear and tear of the spine with age – this is called degenerative scoliosis, which affects older adults
Scoliosis Association UK has more information about the different types of scoliosis.
Marfan syndrome – what are the signs and symptoms of Marfan syndrome?
Symptoms of Marfan syndrome
Marfan syndrome can affect many parts of the body, including the skeleton, eyes, and heart and blood vessels (cardiovascular system).
The severity of the symptoms varies widely. Some people experience a few mild symptoms, whereas others – about 1 in 10 – experience more severe symptoms.
The symptoms of Marfan syndrome tend to get more severe as a person gets older.
Skeleton
Someone with Marfan syndrome may have several distinct physical characteristics. They may be:
tall and slim, with long, thin arms and legs
have loose and very flexible joints
If your child is particularly slim or tall for their age, it doesn’t necessarily mean they have Marfan syndrome. It’s a rare syndrome, and your child will usually have a number of other symptoms if they have it.
Other physical characteristics of Marfan syndrome can include:
a small lower jaw
a high, arched palate (roof of the mouth)
deep-set eyes
a breastbone (sternum) that either protrudes outwards or indents inwards
crowded teeth
Scoliosis
Marfan syndrome can cause the spine to become abnormally curved to the sides. This is known as scoliosis.
Curvature of the spine can cause long-term backache. In severe cases, it can also make breathing difficult as the spine may press against the heart and lungs.
Spondylolisthesis
Spondylolisthesis is where one of the bones in your spine (a vertebra) slips forward over another vertebra.
This usually occurs in the lower spine, and can cause back pain and stiffness. Anyone can develop spondylolisthesis, but it more commonly affects people with Marfan syndrome.
Dural ectasia
The dura is the membrane that lines your brain and spinal cord. Dural ectasia is a condition where the dura becomes weakened and expands outwards.
People with Marfan syndrome are at particular risk of developing dural ectasia. As the membrane expands, it can press on the vertebrae in your lower back, which can cause:
backache
numbness or pain in your legs
Eyes
Many people with Marfan syndrome have some type of vision problem.
Lens dislocation affects half of all people with the syndrome. This is where the eye’s lens, the transparent structure that sits behind the pupil and focuses light, falls into an abnormal position.
Other possible eye-related symptoms of Marfan syndrome include:
myopia – short-sightedness
glaucoma – increased pressure in the eyeball which, left untreated, can cause permanent vision loss
aortic anyurism – where cloudy patches develop in the eye’s lens, causing blurred or misty vision
retinal detachment – where the light-sensitive layer of cells at the back of your eye (retina) begins to pull away from the blood vessels that supply it with oxygen and nutrients
Cardiovascular system
Marfan syndrome can affect the cardiovascular system, which is made up of your heart and blood vessels. It’s particularly serious if your aorta and heart valves are affected.
Aorta
The aorta is the main artery in the body. It runs from your heart, down the centre of your chest, and through your abdomen.
In people with Marfan syndrome, the walls of the aorta are weak. This can sometimes cause the aorta to enlarge and balloon, which is known as an aortic aneurysm.
In severe cases, the aorta can split (rupture), causing potentially fatal internal bleeding.
Valves
Your heart has four chambers that pump blood to and from the rest of the body. To control the flow of blood through your heart’s chambers, your heart has four valves:
mitral valve
aortic valve
tricuspid valve
pulmonary valve
These valves act as one-way gates, allowing blood to flow through in one direction. In some people with Marfan syndrome, the mitral or tricuspid valves don’t close properly and blood leaks back through the valve.
Read more about common mitral valve problems.
The aortic valve may also leak, leading to the main pumping chamber (left ventricle) gradually becoming enlarged.
Monitoring
If your GP thinks you may have Marfan syndrome, you’ll be referred to a specialist for testing. Your heart and blood vessels will be examined for the symptoms of the syndrome.
Read more about diagnosing Marfan syndrome.
Stretch marks
Stretch marks are pink, red, or white streaks in the skin. They can appear when you gain or lose weight quickly, when you have a growth spurt during childhood, or during pregnancy.
People with Marfan syndrome often develop stretch marks because the tissue in their skin is weakened and the skin isn’t as elastic as it should be.
If you have Marfan syndrome, stretch marks are most likely to appear on your:
shoulders
hips
lower back
Over time, they’ll gradually fade to a silvery colour and will be difficult to see.
Scoliosis – what are the signs and symptoms of Scoliosis and how can it be treated?
Some years ago I look a five week course in the Alexander technique to help me relax. The Alexander Technique “teaches people how to stop using unnecessary levels of muscular and mental tension during their everyday activities”. It is often used by people with back problems. Indeed there was a lady in the group who suffered from scoliosis and she hoped that the technique would be of assistance.
This was the first but not the last time that I have come across Scoliosis in my professional and personal life.
Scoliosis is simply an abnormal curvature of the spine. It should be noted that the effects and severity can be very different from person to person.
How common is it? Until recently it was thought that Scoliosis was a condition which developed in childhood. While 0.30% of children are born with Scoliosis it now seems that it may develop in older people but only to a very minor degree.
The causes of Scoliosis really vary but in around 80% of cases they are simply unknown. However people with Marfan syndrome, cerebral palsy, muscular dystrophy and Neurofibromatosis are all at higher risk.
Typical signs of Scoliosis are:-
1) Visible curvature of the spine. The lady at the group I was in did not have this.
2) A tendency to lean to one particular side
3) Clothes not hanging correctly
4) There are some cases of bowel and bladder problems.
Back pain seems to be common with adults with Scoliosis. You can read more about back pain at a previous blog https://patienttalk.org/?p=389.
A lot of children, with mild symptoms, simply grow out of Scoliosis. In some more severe occurrences a back brace can be used to help straighten the spine. Unfortunately this can cause body image issues especially for adolescents. It should be noted that surgery for children with Scoliosis is very rare.
With adults who have back pain various pain killers are often employed.
As well as raising awareness of Scoliosis one of the objectives of this blog post is to provide our readers with a space they can use to share their experiences.
It would be great if you could use the comments box below to tell us a bit about how Scoliosis has impacted you and your family. It would be great if you could consider the following questions:-
a) What were your signs of Scoliosis? At what age was the diagnosis of Scoliosis made?
b) Did you need treatments? How effective were these treatments?
c) Has Scoliosis had any long term effects on your lifestyle?
d) Is there one piece of advice you would give to somebody whose child has been diagnosed with Scoliosis?
There questions are really only suggestions. Anything would want to share about Scoliosis would be of great interest to our readers.
Thanks very much in advance.