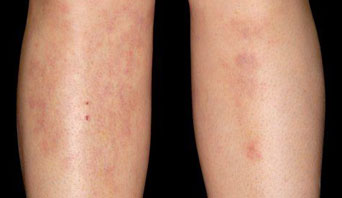
Panniculitis is a broad term referring to inflammation of the fatty layer underneath the skin. It’s usually seen in women, on the thighs and lower legs.
There are many types of panniculitis – with different causes – but the condition generally causes the skin to feel hard and to develop painful red lumps (nodules) or patches (plaques), making it look darker in places.
Panniculitis usually affects the shins and calves, but may spread to the thighs, forearms and chest. It tends to clear up within six weeks, fading like a bruise, usually without scarring.
When the inflammation has settled, a depression in the skin may be left, which can be temporary or permanent.
Many people get recurring bouts of panniculitis.
Other symptoms
As well as skin symptoms, panniculitis may also be associated with:
fever
weight loss
nausea and vomiting
joint pain
What are the causes?
There are a wide range of possible causes of panniculitis, although often the cause is not known. Common causes include:
an infection – usually a viral or bacterial infection, but sometimes tuberculosis
an inflammatory disease such as Crohn’s disease or ulcerative colitis
some medicines, including the oral contraceptive pill or sulphonamides (a group of antibiotics)
sarcoidosis – a rare disease that causes body cells to form into clumps, called granulomas, in the lungs and skin
leukaemia (cancer of the white blood cells) or lymphoma (cancer of the lymphatic system, part of your immune system)
Some cases of panniculitis may be caused by the body’s immune system mistakenly attacking the fat cells.
Types of panniculitis
The layer of fat underneath the skin is made of lobules (groups of fat cells) held together by connective tissue. Doctors sometimes classify the disease as either:
‘mostly septal’ – the inflammation mostly affects the connective tissue
‘mostly lobular’ – it mostly affects the fat lobules
Some people will also have vasculitis, where the immune system attacks the body’s blood vessels. If a blood vessel is inflamed, it can narrow or close off, this can limit, or even prevent, blood flow through the vessel and potentially damage organs.
The most common type of panniculitis is erythema nodosum, which affects the shins. In about half of all cases of erythema nodosum, the cause is unknown.
A similar form of the disease is Weber-Christian disease, also known as idiopathic lobular panniculitis (idiopathic means ‘unknown cause’). This most commonly affects the thighs and lower legs of women aged 30-60, and can also cause the non-skin symptoms mentioned above, such as fever and fatigue.
Other types include:
erythema induratum (nodular vasculitis), which usually affects the calves of young women and is often caused by tuberculosis
cold panniculitis, which affects areas of skin exposed to the cold – for example, it can affect the cheeks and forehead of infants and children
subcutaneous sarcoidosis, when the cause is the rare disease sarcoidosis
A full list of all the different types of panniculitis can be found on DermNet NZ, which provides pictures and detailed information on the specific types.
How is panniculitis treated?
Doctors will aim to treat the underlying cause of the panniculitis, if known, and relieve some of the symptoms. While treatment is underway, you will be asked to ensure you get enough rest and to elevate the affected area when possible.
Treatments will vary; for example, if panniculitis is triggered by medication, this medicine should be stopped – but don’t stop taking any medication without first speaking to your GP.
If the cause is a bacterial infection, you will be prescribed anti-inflammatory antibiotics, such as tetracycline, to clear the infection.
If the cause is sarcoidosis, you may not need any medical treatment as the disease often goes away on its own with time (usually a couple of years). Often, simple lifestyle changes, over the counter painkillers, and support bandages are all that is needed to control any flare ups. Read more about managing sarcoidosis.
The following treatments may help to relieve symptoms:
Joint pain and painful skin nodules can be relieved with anti-inflammatory painkillers such as ibuprofen.
A solution of potassium iodide may help to relieve symptoms – this is thought to have an effect on white blood cells
The inflammation may occasionally be treated with other therapies if the immune system is responsible.
If the condition is severe and the above treatments don’t help, you may wish to consider surgical removal of particularly bad patches of skin. Your GP will refer you to a dermatologist (skin specialist) to discuss the pros and cons of surgery.